Managing diabetes effectively requires consistent glucose monitoring, yet many people struggle with accuracy and convenience. Whether you rely on traditional finger prick testing or newer continuous monitoring technology, establishing a reliable routine transforms diabetes management from reactive crisis handling to proactive health optimisation. This guide walks you through proven methods for routine glucose checking, from selecting the right equipment to interpreting readings and troubleshooting common challenges, empowering you to take confident control of your condition.
Table of Contents
- Understanding Routine Glucose Monitoring Methods
- Preparing For Regular Glucose Checks: Equipment And Setup
- Executing Routine Glucose Testing: Step-By-Step Guide
- Common Challenges And Ensuring Accurate Glucose Monitoring
- Explore Advanced Glucose Monitoring Solutions At EVELOP
- Frequently Asked Questions
Key takeaways
| Point | Details |
|---|---|
| Monitoring frequency varies | Insulin users typically check multiple times daily, whilst others monitor less frequently based on individual treatment plans and diabetes type. |
| CGM offers continuous insights | Real-time glucose tracking reduces hypoglycaemia risk and improves time in target range without increasing dangerous lows. |
| Non-invasive options emerging | Optical and microwave methods show promise but currently have approximately 20% measurement error compared to established techniques. |
| Structured education matters | Combining individualised frequency guidance with ambulatory glucose profile reports significantly enhances monitoring effectiveness. |
| Equipment preparation crucial | Proper storage, calibration, and hygiene practices directly impact result accuracy and reliability. |
Understanding routine glucose monitoring methods
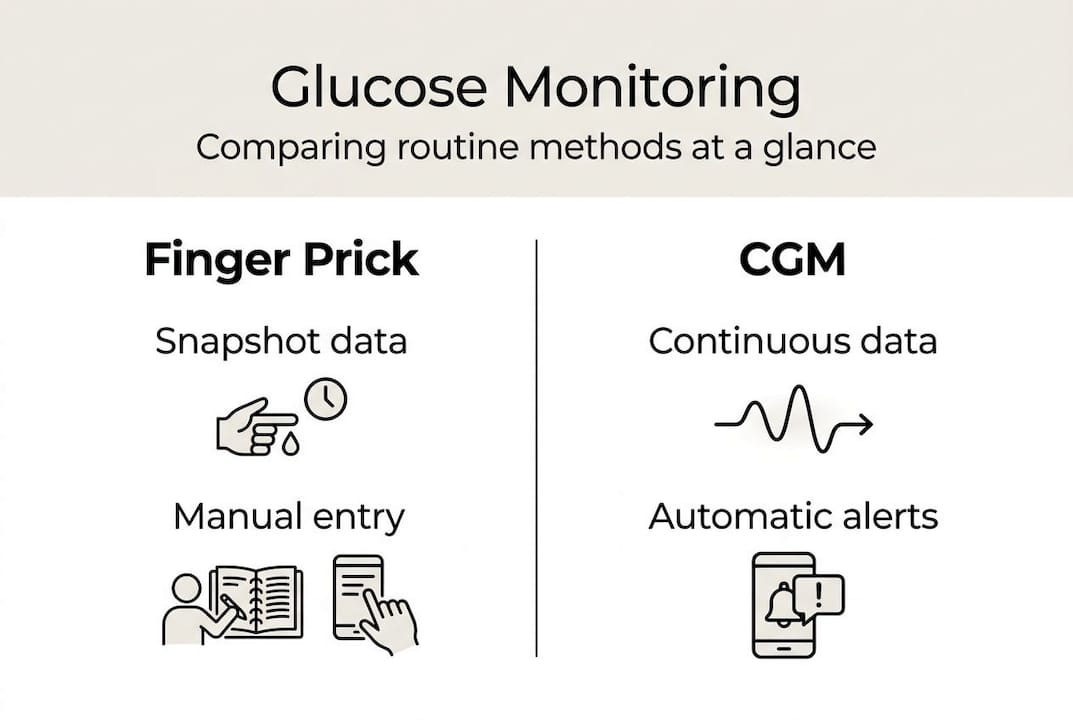
Choosing the right glucose monitoring approach depends on your diabetes type, treatment plan, and lifestyle needs. Routine glucose monitoring for diabetes involves SMBG for intermittent checks and CGM for continuous real-time tracking, with frequency individualised based on insulin use and management goals. Each method offers distinct advantages and limitations worth understanding before committing to a routine.
Self-monitoring of blood glucose uses finger prick testing to capture snapshots of glucose levels at specific moments. You typically test before meals, at bedtime, and during situations that might trigger hypoglycaemia or hyperglycaemia. Whilst SMBG provides accurate point-in-time readings, it misses fluctuations between tests and requires multiple painful finger pricks throughout the day. Many insulin users find the constant testing burdensome, leading to reduced compliance and gaps in data that compromise treatment decisions.
Continuous glucose monitoring revolutionises diabetes management by measuring interstitial glucose levels every few minutes through a small sensor worn on your skin. How continuous glucose monitoring works involves inserting a tiny filament just beneath the skin surface that transmits readings wirelessly to your smartphone or receiver. CGM systems alert you to dangerous highs and lows before they become critical, enabling proactive intervention rather than reactive damage control. Research consistently shows CGM reduces hypoglycaemia episodes and improves time in target range compared to finger prick testing alone.
Emerging non-invasive glucose monitoring research explores optical spectroscopy, electromagnetic sensing, and other technologies that measure glucose without breaking the skin. These methods analyse light absorption, thermal emission, or microwave properties to estimate glucose levels. Whilst appealing for their pain-free approach, current non-invasive devices suffer from accuracy issues, with measurement errors around 20% that make them unsuitable for treatment decisions. Most remain in research phases rather than commercial availability in 2026.
The choice between methods depends on several factors:
- Insulin therapy intensity: Multiple daily injections or pump users benefit most from CGM's continuous data
- Hypoglycaemia awareness: People with reduced warning symptoms need CGM alerts for safety
- Lifestyle flexibility: Active individuals appreciate CGM's ability to track exercise effects without constant finger pricks
- Budget considerations: CGM sensors cost more upfront but may reduce long-term complications
- Personal preference: Some people prefer discrete sensor wear whilst others mind the constant device presence
Understanding cgm versus finger prick testing trade-offs helps you select the monitoring strategy that aligns with your treatment goals and daily reality. Many people combine both methods, using CGM for continuous tracking whilst confirming critical readings with finger prick tests during calibration or when symptoms don't match sensor data.
Preparing for regular glucose checks: equipment and setup
Proper preparation ensures accurate, reliable glucose readings that inform effective treatment decisions. Gathering the right equipment and establishing consistent testing conditions eliminates variables that compromise data quality. Whether you use finger prick testing or CGM, attention to setup details pays dividends in measurement precision and long-term diabetes control.
For self-monitoring of blood glucose, you need a glucometer, compatible test strips, lancets, a lancing device, and alcohol wipes or soap for hand hygiene. SMBG mechanics involve finger prick with a glucometer, recommended before meals, bedtime, and during hypoglycaemia or hyperglycaemia risk periods for insulin users. Modern glucometers require tiny blood samples and provide results within seconds, but accuracy depends on proper strip storage and device calibration.

Continuous glucose monitoring systems include a sensor, transmitter, and receiver or smartphone app. The sensor adheres to your skin, typically on the upper arm or abdomen, and lasts 10 to 15 days depending on the model. You insert the sensor using an applicator that positions the filament beneath your skin in seconds. After a brief warm-up period, the sensor begins transmitting glucose readings continuously. Best cgm for diabetes UK options include features like waterproof design, Bluetooth connectivity, and customisable alert thresholds.
Personal preparation significantly impacts reading accuracy. Always wash your hands thoroughly with soap and warm water before finger prick testing, as residual food or sugary substances on your skin can falsely elevate readings. Dry your hands completely, since moisture dilutes blood samples and causes errors. For CGM insertion, clean the application site with alcohol and allow it to dry fully. Avoid areas with scars, moles, or stretch marks that might interfere with sensor accuracy.
Environmental factors affect glucose monitoring reliability:
- Temperature extremes damage test strips and alter glucometer calibration
- Humidity exposure degrades strip chemistry, causing falsely high or low readings
- Direct sunlight on CGM sensors can create thermal interference
- Altitude changes may temporarily affect interstitial glucose measurements
- Electromagnetic fields near medical equipment sometimes disrupt CGM transmission
| Equipment | Storage requirements | Replacement frequency | Accuracy considerations |
|---|---|---|---|
| Test strips | Room temperature, sealed container | Discard after expiry date | Humidity exposure causes errors |
| Lancets | Clean, dry location | Single use only | Reusing increases infection risk |
| CGM sensors | Original packaging until use | Every 10-15 days | Proper adhesion essential |
| Glucometers | Away from heat and moisture | Battery replacement as needed | Calibrate with control solution |
Pro Tip: Store test strips in their original vial with the lid tightly closed, never in the bathroom where humidity fluctuates. Check expiry dates monthly and discard strips past their use-by date, as expired strips produce unreliable readings that compromise treatment decisions.
Executing routine glucose testing: step-by-step guide
Mastering the technical steps of glucose testing builds confidence and ensures consistent, accurate results. Following standardised procedures reduces user error and creates reliable data patterns your healthcare team can interpret effectively. Whether performing finger prick tests or managing CGM systems, methodical execution transforms monitoring from a chore into an empowering health practice.
Finger prick testing follows a specific sequence:
- Wash hands with soap and warm water, then dry completely
- Insert a fresh lancet into the lancing device and adjust depth setting for your skin type
- Load a new test strip into the glucometer and wait for the ready signal
- Lance the side of your fingertip rather than the pad, rotating fingers to avoid soreness
- Gently squeeze to form a blood droplet without excessive milking that dilutes the sample
- Touch the test strip edge to the blood droplet and wait for the meter to draw sufficient sample
- Read the result after the countdown completes and record it in your logbook or app
- Dispose of the lancet in a sharps container and clean any blood from your finger
Continuous glucose monitoring requires less frequent active testing but demands attention to sensor management. Apply the sensor according to manufacturer instructions, ensuring the adhesive sticks firmly to clean, dry skin. Most systems require a two-hour warm-up period before displaying readings. Once active, sync the sensor with your smartphone app or receiver to view real-time glucose levels, trend arrows showing direction and speed of change, and historical data graphs.
Structured education combining frequency individualisation and use of AGP reports enhances glucose monitoring effectiveness. Ambulatory glucose profile reports compile your CGM data into standardised visual formats that reveal patterns invisible in raw numbers. These reports show your median glucose, time in range, and variability across different times of day. Share these insights with your healthcare provider during appointments to identify opportunities for treatment optimisation.
Responding appropriately to glucose readings prevents complications:
- Hypoglycaemia below 3.9 mmol/L requires immediate action with 15 grams of fast-acting carbohydrate
- Recheck glucose after 15 minutes and repeat treatment if still low
- Once glucose rises above 4.0 mmol/L, consume a small snack with protein to prevent recurrence
- Hyperglycaemia above 13.9 mmol/L warrants checking ketones if you use insulin
- Contact your healthcare team if glucose remains elevated despite correction doses
- Document all episodes with context about food, activity, stress, and illness
CGM alerts notify you of impending problems before they become emergencies. Set threshold alerts for your individual targets rather than default values. Enable predictive alerts that warn when your glucose trajectory will cross thresholds within 20 to 30 minutes. This advance notice allows preventive action, like consuming a small snack to head off hypoglycaemia or taking a correction dose before hyperglycaemia worsens.
Pro Tip: Log your glucose readings alongside meals, exercise, medication doses, and stress levels in a diabetes management app. Patterns emerge over weeks that reveal how specific foods, activities, or situations affect your glucose control. Share this contextualised data with your healthcare team through diabetes and CGM expert guides resources to receive personalised adjustment recommendations.
Common challenges and ensuring accurate glucose monitoring
Even with proper technique, glucose monitoring presents obstacles that frustrate users and compromise data quality. Recognising these challenges and implementing practical solutions maintains measurement reliability and sustains long-term monitoring adherence. Addressing both technical issues and human factors creates a sustainable routine that delivers the insights needed for optimal diabetes management.
Frequent finger prick testing causes physical discomfort that reduces compliance. Fingertips develop calluses, soreness, and occasional infection from repeated lancing. Rotate testing sites across all fingers, using the sides rather than the sensitive pads. Adjust your lancing device to the shallowest depth that produces adequate blood samples. Some people find alternate site testing on forearms or palms less painful, though these locations may lag behind fingertip readings during rapid glucose changes.
CGM sensor accuracy varies based on physiological and technical factors. CGM has a 5-10 minute lag compared to blood glucose and sometimes overestimates postprandial values, requiring calibration and consistent use to avoid inaccuracies. This lag means sensor readings trail actual blood glucose during rapid rises or falls. During exercise or after meals, your CGM might show values that differ from simultaneous finger prick tests by 10 to 20 per cent. Understanding this limitation prevents panic over apparent discrepancies.
Common technical issues include:
- Sensor errors from poor adhesion, compression during sleep, or premature failure
- Glucometer inaccuracies from expired strips, incorrect coding, or inadequate blood samples
- Transmission interruptions between CGM sensors and receivers due to distance or interference
- Battery depletion in devices causing missed readings or lost data
- User errors like applying insufficient blood, contaminated samples, or incorrect timing
| Challenge | SMBG approach | CGM approach |
|---|---|---|
| Pain and discomfort | Rotate fingers, adjust depth, use sides | Rotate sensor sites, secure adhesive |
| Inaccurate readings | Verify strip expiry, clean meter | Calibrate with finger prick when prompted |
| Missing data points | Set testing reminders | Check transmitter battery, maintain proximity |
| Cost management | Buy strips in bulk, check insurance | Explore subscription options, patient assistance |
Verifying measurement accuracy requires periodic comparison between methods. Perform finger prick tests alongside CGM readings when glucose is stable, avoiding times of rapid change. If discrepancies exceed 20 per cent consistently, recalibrate your CGM or contact technical support. Some CGM systems require regular calibration with finger prick values, whilst others are factory calibrated and need verification only when readings seem questionable.
Critical warning: Never ignore severe hypoglycaemia symptoms even if your CGM shows acceptable readings. The sensor lag during rapid glucose drops means you might experience symptoms before the device alerts you. If you feel shaky, sweaty, confused, or dizzy, treat immediately with fast-acting carbohydrate and verify with a finger prick test. Seek emergency medical care for loss of consciousness or seizures.
Reducing pain whilst maintaining accuracy requires balancing comfort with data quality. Warm your hands before finger prick testing to improve blood flow and reduce the pressure needed. Apply sensors to areas with adequate subcutaneous fat and minimal movement to prevent dislodgement. Use skin adhesive products designed for CGM to extend sensor wear time without irritation. Compare cgm versus finger prick testing experiences with others in diabetes communities to discover practical tips that healthcare providers might not mention.
Explore advanced glucose monitoring solutions at EVELOP
Transitioning from traditional finger prick testing to continuous glucose monitoring transforms diabetes management from reactive to proactive. EVELOP specialises in innovative healthcare devices that eliminate the pain and inconvenience of routine testing whilst providing superior data quality. The Sinocare iCan i3 CGM delivers 15 days of continuous, pain-free glucose monitoring with zero finger pricks required. This medical-grade device features waterproof design, Bluetooth connectivity, and customisable alerts that notify you of dangerous glucose excursions before they become emergencies.
Whether you're managing diabetes yourself or supporting a loved one as a carer, EVELOP's CE and FDA certified continuous glucose monitors provide the accuracy and convenience you need for confident diabetes control. Explore the complete range of CGM solutions and expert guidance at EVELOP to discover how advanced monitoring technology simplifies your daily routine whilst improving health outcomes. Pro Tip: Integrate CGM data sharing with your healthcare provider through app connectivity features, enabling remote monitoring and timely treatment adjustments without extra appointments.
Frequently asked questions
How often should I check my glucose levels?
Monitoring frequency depends on your diabetes type and treatment plan. Insulin users typically check four to eight times daily with finger pricks, covering pre-meal, bedtime, and situational testing. CGM users benefit from continuous readings every few minutes without active testing, though some systems require occasional finger prick calibration. Non-insulin users might test once or twice daily or several times weekly based on their healthcare provider's recommendations and glucose stability.
Are non-invasive glucose monitors reliable and available now?
Non-invasive glucose monitoring technologies remain in development stages with limited commercial availability in 2026. Current devices using optical spectroscopy or electromagnetic sensing show approximately 20 per cent measurement error compared to blood glucose reference standards. This accuracy gap makes them unsuitable for treatment decisions like insulin dosing. Minimally invasive CGM with subcutaneous sensors remains the established choice for reliable continuous monitoring until non-invasive technology achieves regulatory approval and clinical validation.
Can caregivers use CGM effectively to support diabetes management?
CGM preferred for insulin users and caregivers enables proactive management, reducing hypoglycaemia risk and improving time in range without increasing dangerous lows. Caregivers receive real-time glucose data and alerts on their smartphones, allowing remote monitoring of children, elderly parents, or partners with diabetes. This capability provides peace of mind during school, work, or overnight hours whilst enabling timely intervention when glucose levels become concerning. Data sharing features let multiple caregivers coordinate responses effectively.
What common mistakes should I avoid when checking glucose?
Frequent errors include testing with unwashed hands contaminated by food residue, which falsely elevates readings. Applying insufficient blood to test strips causes inaccurate results, as does using expired strips or improperly stored supplies. Many people forget to calibrate CGM sensors when prompted or ignore device alerts about sensor issues. Inconsistent testing times prevent pattern recognition that guides treatment adjustments. Following manufacturer instructions carefully and participating in structured diabetes education programmes significantly reduces these mistakes and improves monitoring effectiveness.
